New Patients
(865) 876-7050
Existing Patients
(865) 947-2220
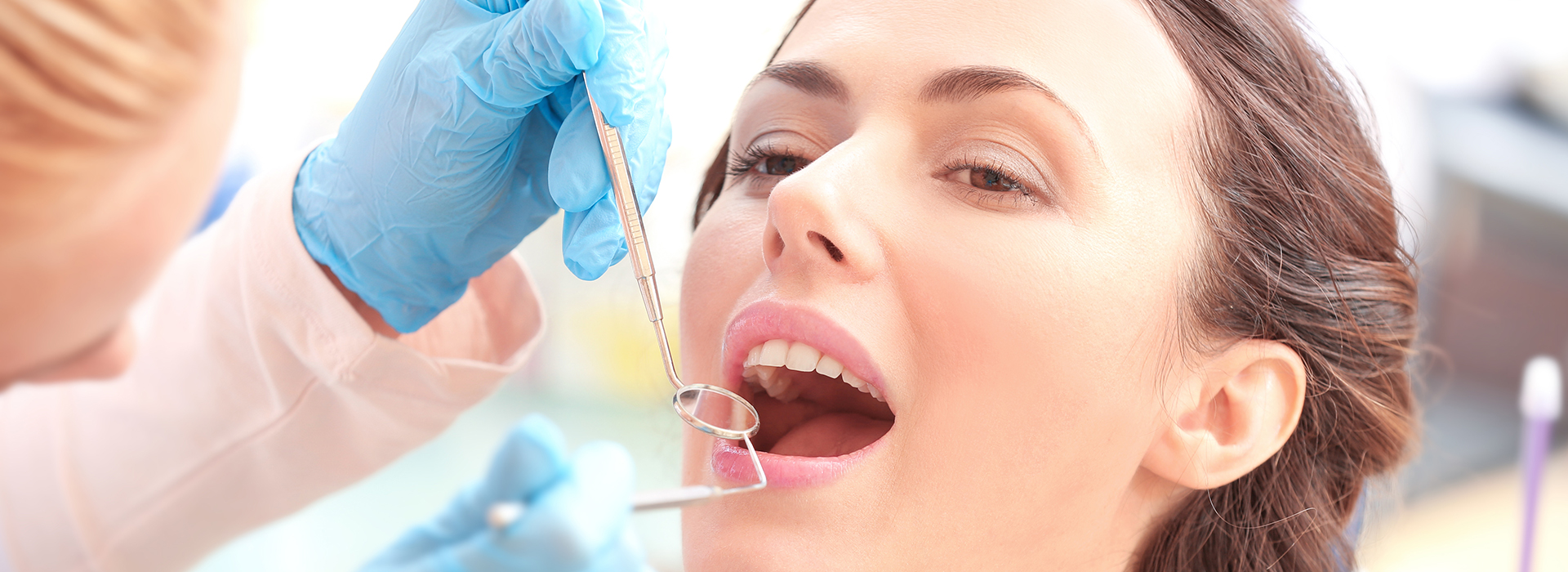
Gum disease is one of the most common threats to adult oral health. Studies show that a large portion of adults experience some level of periodontal infection by age 30, and many cases progress quietly for years. At Kennedy Dentistry, we focus on early recognition and effective management so patients can keep their natural teeth and maintain overall health.
Periodontal disease begins when bacterial plaque accumulates along the gumline. Left in place, this sticky film hardens into tartar and creates an environment where bacteria can irritate and inflame gum tissue. That inflammation is the body’s response — but over time it damages the structures and bone that anchor teeth.
Because early stages are often painless, many people don’t notice a problem until the condition is more advanced. Regular dental checkups let your dental team detect subtle signs — pocketing, bleeding, or changes in gum contour — before irreversible harm occurs. Prevention and early intervention are the most predictable paths to long-term stability.
Understanding how plaque, tartar, and inflammation interact helps explain why routine home care and professional cleanings are essential. Brushing and flossing disrupt plaque, while periodic periodontal maintenance addresses deposits below the gumline that home care cannot reach.
Red, swollen, or tender gums
Bleeding during brushing or flossing
Notable gum recession or exposed tooth roots
Increased sensitivity to temperature or sweets
Persistent bad breath or an unpleasant taste
Tooth mobility or a sensation that teeth no longer fit together as they used to
New gaps appearing between teeth
Partial dentures that feel loose or misfitting
Pus or discharge around the gumline
Discomfort when biting or chewing

Oral health and overall health are closely linked. Persistent gum inflammation is associated with increased systemic inflammation, which researchers have connected to cardiovascular disease, diabetes control, and respiratory conditions. Managing periodontal infection reduces local damage and can lessen inflammatory burden that affects the rest of the body.
When we evaluate patients, we consider the whole person — medical history, medications, smoking status, and systemic conditions that influence healing. This holistic approach guides treatment choices and helps us prioritize interventions that support both oral and general wellness.
Preventive steps — consistent home care, professional cleanings, and early periodontal therapy when needed — are simple, evidence-based actions that protect teeth and reduce risk factors linked to broader health concerns.
Gingivitis is the earliest, reversible form of periodontal disease. It shows up as inflamed, tender, or bleeding gums but does not yet damage the bone or connective tissues that hold teeth in place. Because the underlying structures remain intact, timely treatment can restore healthy gums without surgery.
Typical first-line responses include a focused cleaning, instruction to improve brushing and flossing techniques, and a short course of more frequent monitoring. We emphasize practical, sustainable habits patients can adopt so improvements last beyond the dental chair.
With gingivitis, commitment matters: consistent daily care plus regular professional oversight typically returns the tissue to a healthy state. If early treatment is neglected, gingivitis can transition into a more destructive phase requiring more involved care.

When inflammation progresses beyond gingivitis, it becomes periodontitis. At this stage, the infection affects connective tissue attachments and the jawbone supporting teeth. Pocketing develops as gum tissue separates from root surfaces, and bone loss can follow — changes that can compromise tooth stability if left untreated.
Treatment for periodontitis aims to halt disease activity and preserve as much of the natural support system as possible. That often begins with deeper cleaning below the gumline to remove bacterial deposits and minimize pocket depth. In many cases, adjunctive therapies are used to reduce bacterial load and encourage tissue healing.
Where structural damage is significant, regenerative strategies such as bone grafting or guided tissue regeneration may be recommended to rebuild lost volume and improve the prognosis for affected teeth and future restorative work.
Over the past decade, periodontal care has evolved to include targeted surgical techniques, minimally invasive laser-assisted procedures, and biologic materials that support tissue regeneration. These tools expand options for repairing damage, improving function, and enhancing appearance when gum recession or bone loss has occurred.
For patients who require tooth replacement, modern implant protocols combined with periodontal therapy can restore chewing ability and esthetics. Successful outcomes rely on controlling infection first, then planning restorative steps that respect the health of surrounding tissues.
Every treatment plan is tailored. Our goal is to use evidence-informed methods to stabilize disease, restore healthy anatomy where possible, and create a maintenance schedule that protects results over time.
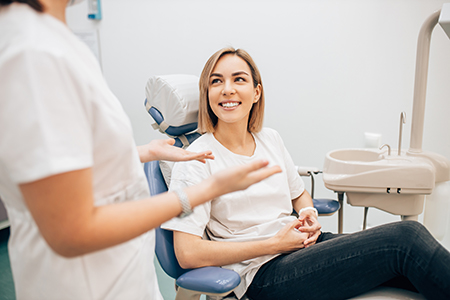
Choosing the appropriate therapy begins with a comprehensive assessment: clinical measurements of pocket depth, charting of attachment levels, digital imaging when indicated, and a review of health factors that influence healing. That information helps us stage the disease and explain realistic outcomes for each option.
In many cases, non-surgical care such as scaling and root planing, combined with improved home hygiene and localized antimicrobial therapy, can control infection and reduce pocketing. These approaches are effective when disease is detected before extensive structural loss occurs.
If pockets are deep, bacteria persist despite conservative care, or there is significant bone loss, surgical intervention may be recommended to thoroughly clean root surfaces, reshape supporting tissues, and, when appropriate, place regenerative grafts. Modern periodontal surgery aims to be precise and to support long-term maintainability.
Early-stage and moderate disease are often managed without surgery. Scaling and root planing remove deposits beneath the gums and smooth root surfaces to discourage bacterial recolonization. In-office debridement may be paired with targeted antimicrobial agents placed locally or prescribed systemically when indicated to reduce bacterial burden.
After initial therapy, a personalized maintenance program — typically more frequent cleanings and focused home-care strategies — helps stabilize the gums and prevents recurrence. This conservative path preserves tissues and is the least invasive route to disease control when it is effective.
Patient participation is essential: successful non-surgical care depends on daily oral hygiene practices and adherence to scheduled periodontal maintenance visits.
If conservative measures do not sufficiently reduce pocket depths or inflammation, we reassess and discuss surgical options to achieve lasting control.
Surgery becomes a recommended step when pocketing or tissue destruction prevents adequate cleaning and stabilization by non-surgical means. The objectives are to remove diseased tissue, reduce pocket depth, and recontour bone and gums to facilitate long-term cleaning and maintenance.
Flap procedures allow clinicians to access and clean root surfaces thoroughly and to reshape supporting structures. When regeneration is possible, bone grafts and biologic membranes can encourage new tissue formation and improve support.
Contemporary surgical care may also incorporate laser therapy for select cases, which can reduce bacterial levels and reshape soft tissue with controlled precision. When combined with good post-operative care and ongoing maintenance, surgical treatment can significantly reduce the risk of tooth loss.
Eliminate subgingival bacterial reservoirs on root surfaces
Protect remaining bone and, when feasible, rebuild lost volume
Decrease pocket depth so daily hygiene and professional maintenance are more effective
Keeping gums healthy is a long-term commitment that blends skilled dental care with effective daily habits. If you have concerns about bleeding gums, looseness, or changes in your bite, we encourage you to contact us for more information and an evaluation. Our team is ready to explain your options and help you protect your oral and overall health.
Most people don’t realize that periodontal disease is the leading cause of tooth loss among adults. According to statistics from the Centers for Disease Control and Prevention, one out of every two adults over the age of 30 in the United States has periodontal disease.
You may be surprised to learn that the human mouth is home to a wide variety of microbes. The fact is that over 700 different strains of bacteria have been detected in the oral cavity. Although some of these bacteria are beneficial, others are harmful to oral health. Without proper oral hygiene and routine dental care, these harmful bacteria can cause tooth decay and gum disease, compromising both your oral health and overall wellbeing.
In addition to inadequate oral hygiene and infrequent professional care, other factors, including smoking, genetic tendencies, and unchecked diabetes, can contribute to the escalation of periodontal disease.
Your gums and teeth have an interdependent relationship, which means healthy teeth depend on the support of healthy gums. Also, taking care of your smile does more than keep your teeth and gums in optimal condition; good oral health also supports systemic health. In addition to being the leading cause of tooth loss in adults, researchers are finding more and more links between periodontal disease and a number of medical problems, including heart disease, stroke, diabetes, respiratory problems, and adverse pregnancy outcomes such as pre-term and low birth-weight babies.
If you notice that your gums are bleeding with the slightest pressure while brushing or flossing, it’s a sign of gingivitis. Although gingivitis is the earliest stage of gum disease, it can easily be reversed with deeper cleanings as well as an improved regimen of oral hygiene at home.
In the absence of professional treatment and better home care, gingivitis progresses to the next stage, which is known as periodontitis. In this stage, the connective tissue and bone that hold the teeth in place begin to break down with an increase in pocketing between the teeth and bone, gum recession, and bone loss. Without proper treatment by your dentist, periodontitis will progress from a mild to moderate loss of supporting tissue to the destruction of the bone around the teeth.
Although gingivitis can often be reversed with improved oral hygiene and professional cleanings, as periodontal disease advances, more extensive procedures are required to halt its progression. Based on a complete assessment of your periodontal health and a review of possible contributing factors, our office will recommend the best options in care. Treatment for periodontitis may include a series of deeper cleanings known as root planing and scaling, surgical procedures to reduce pocket depth, bone or tissue grafts, laser procedures, or antimicrobial medications.
The cost of care depends on the type of procedures required to restore your periodontal health. If you have dental insurance, plans often cover treatment to prevent gum disease as well as many procedures to treat the various stages of gum disease. Our goal is to help patients restore and maintain good oral health. We do all we can to help you begin care without additional stress or delay. Our business office works with you to maximize your benefits and provide easier, more convenient payment options.
By seeing our office regularly for care and doing your best to eat a healthy diet and practice good oral hygiene, you can keep your smile in tip-top shape as well as protect your overall wellbeing.
At the office of Kennedy Dentistry, we provide a comprehensive range of services to address all your oral healthcare needs. You can rest assured that your smile is in the best of hands at our office. Our skilled and experienced team maintains a position at the forefront of advances in care and remains dedicated to providing the highest quality of skilled and compassionate treatment.
